Epiploic Appendagitis
What Is Epiploic Appendagitis, What Causes It, And How Is This Condition Diagnosed And Treated?
Epiploic appendagitis, also referred to as appendicitis epiploica or epiplopericolitis is the inflammation or torsion of one or a couple of the hundred or so small protrusions of fatty tissue on the outside wall of the large intestine or colon. It is a common cause of sudden onset abdominal pain often mistaken for appendicitis and other conditions. Find out how to differentiate this condition from other causes of abdominal pain and how it is treated here.
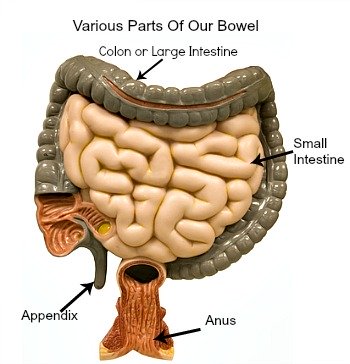
On the outside wall of our colon or large intestine, there are about 100 or so protrusions made up of fat and tissues covering the colon.
They could be as small as half a centimeter to three centimeters in length on the average, pointing perpendicularly away from the colon. These structures are an out-pouching on the outside wall of the bowels, whose function or purpose remains unknown. They are referred to as epiploic appendage.
In some individuals, they have been reported to be as long as 15cm! They have blood vessels supplying nutrient to them.
If for any reason they become inflamed from the spread of a bowel infection or twist along their long axis or if their blood supply gets blocked, they could cause a great deal of abdominal pain.
What Are The Causes Of Epiploic Appendagitis?
As mentioned above, one of three events could lead to the development of inflammation of the epiploic appendage, or appendicitis epiploica. These are:
Appendicitis epiploica arising from torsion of the appendix epiploica, or blood vessel blockade or kinking are referred to as primary appendagitis, while those arising from spread of infection or inflammation somewhere else are referred to as secondary appendagitis.
Symptoms Of Epiploic Appendage Infection
Epiploic appendagitis is not a newly described or recognised disorder. Contrary to what some in the medical field thinks, it is not "only recently been recognized".
It is believed to have been first recognized and reported in the 1850s. The name epiploic appendagitis was first used in 1956 by Lynn et al to describe this condition.
There has been numerous reference to this condition ever since and for some reasons, many doctors have not embraced this important, though relatively uncommon cause of abdominal pain.
It is estimated that for every 100 diagnosis of appendicitis made, one of such cases is actually due to appendagitis and for every 100 cases of suspected diverticulitis, up to 7 are due to inflammation of the epiploic appendage.
The most common symptom of epiploic appendagitis is that of an acute lower right or left abdominal pain. Sometimes, patients with this condition could also develop a upper right side abdominal pain.
Over half (53%) of epiploic appendagitis occurs on the lower left abdominal region.
Conditions that can be mimicked by appendicitis epiploica include:
- Diverticulitis
- Acute Appendicitis
- Cholecystitis
- Omental Infarction
- Mesenteric Panniculitis
If you develop sudden onset upper or lower right or left side abdominal pain and have had tests and all the blood results and scans came back normal, epiplopericolitis could be the cause.
How Is This Condition Diagnosed?
The diagnosis of appendicitis epiploica is usually made from a combination of the story or history given by the patient of:
- Lower left abdominal pain which may be of gradual or sudden onset or
- Lower right abdominal pain resembling that of appendicitis or
- Upper right or left abdominal pain
- Severe pain, but usually without fever (though a very mild fever has been reported in a number of patients diagnosed with this condition), nausea or vomiting and
- All other common causes of abdominal pain has been excluded
- Blood and urine tests normal including normal white blood cells
- Ultrasound scan normal
- CT scan could be reported to be normal, if the radiologist did not actually look out for the CT signs of epiplopericolitis.
The diagnosis is usually made on CT scan, though in the past this condition is only diagnosed either during operation to remove a supposed bad appendix or at laparoscopy. The main findings on CT scan include fat inflammation around the colon, stranding of anti-mesenteric fat without associated bowel wall thickening. In many cases, these signs would be seen if a previously reported CT scan is reviewed.
The CT Scan Findings In Epiploic Appendagitis
|
"As CT scans are increasingly being used for the evaluation of acute abdomen,
radiologists are likely to see acute epiploic appendagitis and its
mimickers more often. Recognition of these conditions on CT images will
allow the appropriate management of the true cause of an acute abdominal pain and may help to
prevent unnecessary surgery." - Radiographics, a scientific journal of radiology of November - December 2005
Where facilities for a CT scan does not exist, an abdominal ultrasound scan may show an "oval hyperechoic mass surrounded by a hypoechoic rim, without Doppler flow", reports the Canadian Medical Association Journal, CMAJ. 2010 June 15; 182(9): 939.
Treatment of Appendicitis Epiploica
Epiploica appendagitis is usually a self limiting condition - that means that it gets better on its own, without the need for any treatment.
Once the diagnosis of this condition is made, treatment involves the use of anti-inflammatory painkillers like ibuprofen or Naproxen and adequate fluid replacement through intravenous drips if severe and rest.
Because appendagitis epiploica does not require treatment in most cases, it is therefore very important to make the right diagnosis and avoid unnecessary bowel surgery with its potential risks.
Very rarely, an inflamed epiploic appendage may develop abscess, needing intravenous antibiotics and in very small cases, surgery. Such cases are so remotely rare enough that it is only mentioned here for completeness sake.
References:
- Baadh AS,Singh S,Graham RE. A Mysterious Cause of a Surgical Abdomen. The Journal of Emergency Medicine, 07 August 2012, 0736-4679.
- Philippe Leclercq, MD and Laurent Dorthu, MD. Epiploic appendagitis. CMAJ. 2010 June 15; 182(9): 939. doi: 10.1503/cmaj.090791.
- Textbook: Practical Differential Diagnosis in CT and MRI By Eugene C. Lin, Edward J Escott, Kavita D Garg. Chapter 103, Page 236. Publication Date: June 18, 2008. ISBN-10: 1588906558.
- Simren Sangha, Jorge A. Soto, James M. Becker, Francis A. Farraye. CASE REPORT: Primary Epiploic Appendagitis: An Underappreciated Diagnosis. A Case Series and Review of the Literature. Digestive Diseases and Sciences. February 2004, Volume 49, Issue 2, pp 347-350.
- Uptodate.com
Last Updated: 18th January 2017.
Think You Might Have Epiploic Appendage Inflammation? Share Your Experience
Had a sudden onset upper or lower quadrant abdominal pain recently and had blood tests, scans etc and told nothing was found? Are you one of the few lucky ones to be told you had epiploic appendage inflammation, thus avoided an unnecessary surgical operation, or perhaps do you think this condition might be the cause of your abdominal pain? We would love to hear from you. Share your experience with other readers here!
What Other Visitors Have Said
Click below to see contributions from other visitors to this page...
Epiploic Appendagitis: My Personal Experience 




I started having pain in my right abdomen on a Thursday and thought I must have strained a muscle somehow.
On Friday morning, the pain was much worse …
pain is a 10 




I was diagnosed this EA about a year ago, it did go away in about 3 months. Now its back and its worse than ever. Just had another CT scan due to the …
epiploic appendagitis is perplexing 




It seems I followed all the symptoms of diverticulitis until a CT scan showed it was Epiploic Apendagitis. It is frustrating waiting to heal on its own …
HELP, BUT NOONE WILL 




I HAVE HAD PAIN FOR TWO MONTHS, FEVER, SWEATING, SICK ON MY STOMACH, CANT HARDLY EAT NOW WITH OUT GETTING SICK, I HAVE LOST WIEGHT, HAD HAVE HEADACHE, …
I was just diagnosed via CT scan 




I have it according to my doctor.
We first assumed it was Diverticulosis...but no. The pain has since gone away with no treatment.
BUT after reading …
Epiploic Appendagitis Diagnosed After Symptoms Of Appendicitis Developed Not rated yet
I had all of the symptoms of appendicitis but because my appendix had been removed over 40 years ago, this could not be the case.
The hospital was …
Diagnosed with Epiploic Appendagitis Not rated yet
I felt a bit nauseous for a week, off and on, then one day I woke up with severe pain in my appendix area. I didnt have Diarrhoea nor vomiting, but when …
Have had on appendectomy as a teenager and at 54 yo felt the same symptoms at the left lower abominal quadrant Not rated yet
Woke 3 days ago with acute pain at the left lower abdominal quadrant and had to urinate badly. Had pain on my left side as I got out of bed and walked …
this is my experience with the known Epiploic Appendagitis /hernia found Not rated yet
Well all my severe pain started over a week ago and my stomach look like it was swelling and getting bigger and felt real hard to the touch .
i had to …
My story--with epiploic appendagitis Not rated yet
I had severe lower right quadrant pain several months ago.Went to clinic and they thought I had appendicitis. I was adamant I did not.
CT scan revealed …
Epiploic Appendagitis: Painful, Not Fun! Not rated yet
Just diagnosed with Epiploic appendagitis today 10/14/16.
Had pain for 2 days and I'm doing a long bike ride this weekend (170 miles), so wanted to …
My experience with this condition called Epiploric Appendagitis Not rated yet
Approximately a month ago, I hired a personal trainer and began a regular workout schedule to strengthen my core then suddenly,I noticed a slight discomfort …
Experience With Developing Epiploic Appendagitis Not rated yet
I developed a slight pain on my let side about 6 days ago, as the day went on it got worse.
By Sunday morning it hurt to walk, yawn or just any movement …
Was it Omental Infarction Not rated yet
I was driving my car sitting in one spot for over an hour in heavy traffic,
after getting out of my car within five minutes I started getting a pain right …
Epiploic Appendagitis: Not Kidney Stones! Not rated yet
Had severe pain in left side.
Urgent care sent me home with a strainer and told me to go to er during the night if pain became unbearable - diagnosis …
My experience with epiploic appendagitis diagnosis and treatment Not rated yet
I was just diagnosed with epiploic appendagitis by CT scan after 10 days of chronic right-sided pain.
I have had diverticulitis for many years, even …
My advice from my experience with epiploic appendagitis Not rated yet
I was just diagnosed with epiploic appendagitis by CT scan after 10 days of chronic right-sided pain.
I have had diverticulitis for many years, even …
Could this be Epiploicitis Appendagitis Not rated yet
For over a year, I have been experiencing pressure behind my left rib cage.
Recently it became worse and more consistent within a week. I finally went …
My experience with Epiploic Appendagitis Not rated yet
Early August 2010 I developed sudden Lower Left abdominal pain, had a CT scan, and was diagnosed with Epiploic Appendagitis.
My doctor of 30 years, …
My experience with this condition called epiploic appendagitis. Not rated yet
I was diagnosed with ea.
Here's my question though - my white blood cell count was through the roof.
I was told it was an appendicitis and prepare …
Epiploic appendagitis causing severe lower left side abdominal pain Not rated yet
I went to the ER in the middle of the night because the pain was too severe to sleep.
When I checked in, the doc thought it might just be constipation …
Appendectomy to hemi-colectomy due to goblet cell carcinoid Not rated yet
I am in severe pain all the time.
For the last 4 years I was in and out of the ER until one day they said that my appendix was inflamed.
They took …
Epiploic Appendagitis Experience Not rated yet
I was sick for a couple of days with diarrhea and then I all of a sudden got this pain in my lower left abdomen.
The pain would not subside so I went …
My doctor just called with my CAT scan results! Not rated yet
Started with chills and fever on Sunday, March 29.
Temps up to 101.8 over the next few days, no diarrhea, just bloated feeling and loss of appetite …
My experience with Epiploic Appendagitis began with slight pain Not rated yet
I had slight abdominal pain from lower right to lower left that started on a Tuesday.
I assumed it was gas associated with IBS which I have had for …
a Tumor Not rated yet
I developed lower right abdominal pain about 6 weeks ago that has steadly gotten worse. I do not have any other symtoms but since the pain is getting worse …
Please help WITH THIS ABDOMINAL PAIN Not rated yet
Please help me, my daughter is 30 weeks pregnant, has had severe upper/mid left abdo pain for nearly two weeks, respite of two days over the past week. …
Epiploic Appendagitis knowing what the issue is. Not rated yet
my husband is still having pain,3-10.
after all the tests,every test imaginable,still no diagnosis,still having pain....my thought today,taking him …
The unimaginable pain Not rated yet
Since 2005 I have been having right side abdominal pain I have done a laparoscopy and I was told that I have an addition and it was corrected as i was …
could this be epiploic appendagitis or what Not rated yet
Iam 72 ,female, 18 st, diabetic , and asmatic.
For about a year i have had sudden pain that lasts 10/20 minutes, in my upper abdominal area. sometimes …
|
Help Keep This Site Going |

Return To Causes Of Abdominal Pain Page From Epiploic Appendagitis Page